Rationale:
Implementation of antiretroviral treatment guidelines, which emphasize maximal and durable suppression of viral load for the majority of individuals infected with HIV, has resulted in a substantial decline in morbidity and mortality. However, many asymptomatic patients are not at immediate risk of serious opportunistic diseases, the effectiveness of antiretroviral therapy wanes over time due to HIV drug resistance, and there are both short- and long-term toxicities of treatment. This motivates a comparison of two strategies, one which conserves treatments by deferring their use while the risk of opportunistic disease is low and one which aims for sustained virologic suppression irrespective of disease risk.
Purpose:
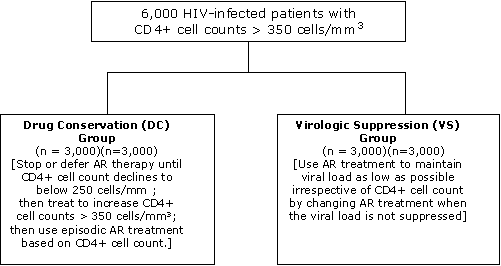
The purpose of this study was to compare the long-term clinical consequences of two strategies of antiretroviral (AR) management:
• the drug conservation (DC) strategy, a strategy aimed at conserving drugs through episodic use of antiretroviral treatment for the minimum time to maintain CD4+ cell count >250 cells/mm 3.
versus
• the viral suppression (VS) strategy, a strategy aimed at suppressing viral load as much as possible, immediately following randomization and throughout follow-up, irrespective of CD4+ cell count.